- Pneumonia is a respiratory condition where a virus, bacteria, or fungal pathogen causes infection and inflammation in the lungs.
- There are two primary forms of pneumonia: community acquired pneumonia (CAP) and hospital acquired pneumonia (HAP).
- Treating pneumonia usually requires supportive therapies such as fluids and, where appropriate, antibiotics, antivirals, or antifungals.
In 2018, around 1.5-million people received a pneumonia diagnosis after visiting the emergency room. Pneumonia can arise following exposure to certain pathogens. In some cases, it occurs when someone aspirates bodily fluids during periods of unconsciousness.
Pneumonia is usually split into two types: community acquired pneumonia (CAP) and hospital acquired pneumonia (HAP). The condition is more severe in very young children, older adults, and immunocompromised patients.
Most people recover from pneumonia, but it can prove fatal and is often preventable. While it’s not possible to prevent pneumonia, certain vaccines and treatments can reduce its severity and the risk of complications.
Pneumonia Symptoms
Classic pneumonia symptoms include:
- Coughing
- Green or blood-stained sputum
- Breathlessness
- Rapid breathing
- Rapid heart rate
- Fever
- Tiredness
- Poor appetite
- Muscle aches
Very young children may experience less-specific symptoms, such as abdominal pain.
Pneumonia Causes
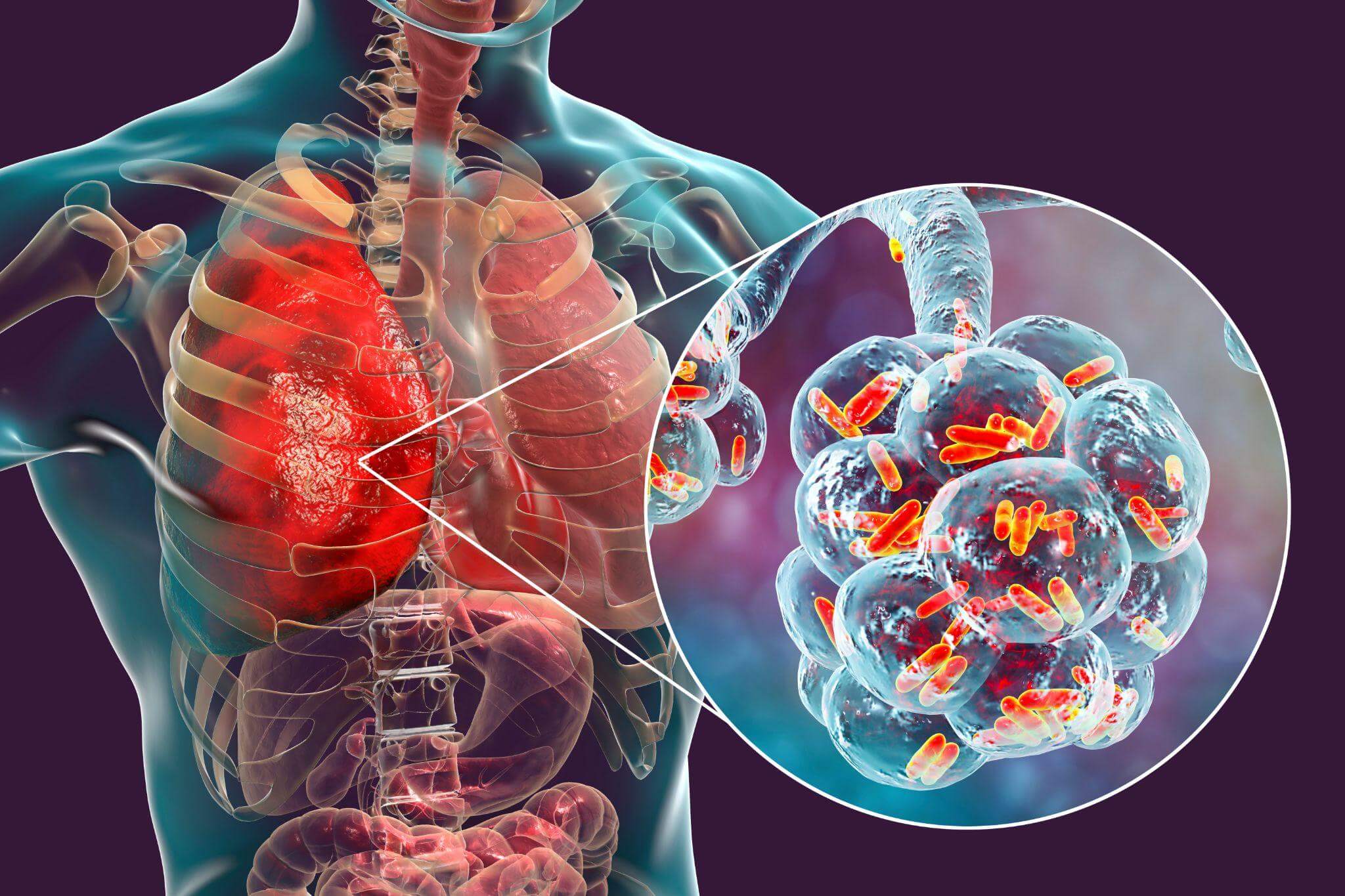
Pneumonia is usually caused by a virus or bacteria. In rare cases, there’s a fungal cause.
Viral Pneumonia
Just under 25 percent of CAP cases have a viral cause. Viruses that can cause pneumonia include:
- Influenza
- Respiratory syncytial virus (RSV)
- SARS-Cov-2
- Adenovirus
- Chickenpox
- Measles
- Whooping cough
Bacterial Pneumonia
Around 14 percent of pneumonia cases are bacterial. Bacteria that can cause pneumonia include:
- Streptococcus pneumoniae
- Mycoplasma pneumoniae
- Chlamydia pneumoniae
- Psittacosis
- Legionella pneumophila
Fungal Pneumonia
Fungal pneumonia is extremely rare in adults who are otherwise healthy. It’s more likely to affect those who have a low immune system due to AIDS, corticosteroid treatment, or chemotherapy.
Some of the fungi that can cause pneumonia include:
- Pneumocystis jirovecii
- Coccidioidomycosis
- Histoplasmosis
- Cryptococcus
Pneumonia Risk Factors

Not all risk factors are modifiable, and certain people are more at risk than others of developing pneumonia. Risk factors for pneumonia include:
- Age. Very young children under the age of five and adults over 65 are more likely to develop pneumonia. Older people are usually at higher risk as the immune system weakens with age.
- Lifestyle. Smoking can make it harder for lungs to clear viruses. Heavy alcohol use weakens some of the body’s defense systems, making CAP more likely.
- Respiratory disorders. Asthma, COPD, and other respiratory disorders can make pneumonia more likely.
- Compromised immune system. Certain drugs and medical conditions suppress the immune system, making it easier for viruses and bacteria to proliferate.
- Drug use. IV drug users have a higher risk of developing pneumonia and are more likely to be hospitalized if they do.
- Hospitalization. A hospital stay or recent hospital discharge can make HAP more likely.
- Neurological disease. Neurological diseases such as Parkinson’s can increase the risk of aspiration pneumonia.
- Chronic diseases. Certain chronic diseases can predispose a person to pneumonia, including diabetes and cardiovascular diseases.
Pneumonia Diagnosis

When diagnosing pneumonia, doctors start by taking a thorough medical history. They’ll also look for certain signs, including the following:
- Vital signs. A fever of 105 degrees, a rapid heart rate, and fast breathing are all common with pneumonia.
- Lung sounds. Using a stethoscope, doctors listen for lung sounds that indicate pneumonia. In some cases, the sounds they hear can suggest which type of pneumonia is present.
- CURB-65. The CURB-65 score is an assessment tool that indicates whether hospitalization is needed for CAP. It assesses vital signs, consciousness levels, and certain blood markers.
- Blood tests. Blood tests can indicate the severity of pneumonia, such as measuring C-reactive protein (CRP). PCR tests can also indicate the type of pneumonia present.
- Sputum tests. Sputum tests can show the type of pathogen present, which is useful for prescribing specific antibiotics.
- X-rays. X-rays aren’t always necessary, but a doctor may request one if the pneumonia appears severe. X-rays are useful for identifying complications.
In HAP cases, your provider may need to repeat tests to assess whether the condition is getting better or worse.
Pneumonia Complications
Each year, around 40,000 people who develop pneumonia die, and many who recover develop complications.
The complications of pneumonia can include:
- Septic shock. Septic shock is a condition where a localized infection spreads to the rest of the body. Without rapid treatment, it can prove fatal. Septic shock is fatal for around 51 percent of those who develop it.
- Kidney failure. A common complication of septic shock is kidney failure. As the kidneys try to cleanse the body of toxins, they may stop working.
- Lung abscesses. In some cases, a pocket of pus may develop and form an abscess.
- Pleural effusion. When pneumonia goes untreated, fluid may gather in the pleura — the layer of tissue that allows lungs to move freely. When this happens, breathing can feel difficult.
- Empyema. Untreated pneumonia may also result in an empyema, or pockets of pus in the pleura. Empyemas make breathing difficult and painful.
- Poor gas diffusion. New evidence demonstrates that pneumonia resulting from COVID-19 may make it difficult for gasses to transfer during breathing. This can result in fatigue.
- Respiratory failure. Respiratory failure is a condition where breathing without assistance becomes challenging. It happens when the lungs fill up with too much fluid.
- Heart failure. Around 12.7 percent of people who require hospitalization due to pneumonia may develop heart failure.
Pneumonia Treatment
The type of treatment used for pneumonia depends on the causative bacteria and how severe it is.
Treatment options can include:
- Antipyretics. Over-the-counter drugs such as acetaminophen (Tylenol), ibuprofen (Motrin and Advil), and aspirin can all reduce fevers. Always seek medical advice if you have an underlying condition.
- Fluids. Staying well-hydrated loosens secretions and makes it easier to bring up phlegm. In hospitals, doctors may use IV fluids.
- Fluid reduction. When fluids gather on the lungs, it’s sometimes necessary for a doctor to aspirate them.
- Antibiotics. Antibiotics are appropriate for bacterial infections. Doctors may use broad-spectrum antibiotics, such as azithromycin or doxycycline.
- Antifungals. Antifungals, such as fluconazole, are often prescribed for fungal cases.
- Antivirals. Most cases of viral pneumonia clear up on their own. However, antivirals, such as zanamivir, can reduce the duration of the illness.
- Oxygen. When blood oxygen levels are too low, hospital admission with oxygen therapy may become necessary.
Pneumonia Prevention

A combination of self-care, good hygiene, and preventative vaccines can prevent pneumonia and reduce its severity.
Vaccines
Vaccines can prevent some cases of pneumonia and make it less severe.
Available vaccines include:
- Pneumococcus. Pneumococcus is a common bacteria that causes pneumonia. Children under the age of two, adults over 65, and immunocompromised patients should get the vaccine.
- Influenza. A seasonal flu vaccine in September or October can prevent pneumonia or reduce its complications.
- Hib. The haemophilus influenzae type B vaccine is recommended for all children under the age of five.
Hygiene
Practicing good hygiene is especially important during the winter months due to an increase in diseases.
Top tips include:
- Hand washing. Wash your hands thoroughly after using the bathroom or coming into contact with an infected person. Consider carrying sanitizing gel and using it too.
- Sneezing. Sneeze into the crook of your elbow to prevent pathogens from spreading.
- Coughing. Always cover your mouth when coughing and wash your hands afterward.
- Social distancing. If you’re aware that someone has a cold, stay away from them until you feel they’re no longer infectious.
Lifestyle
Making the right lifestyle choices can reduce your risk of many illnesses, including pneumonia.
Healthy habits include:
- Exercise. Regular physical activity can boost your immunity.
- Healthy eating. Eat a healthy and balanced diet to keep your immune system strong.
- Quit smoking. Quitting smoking and vaping will make it easier for your lungs to clear pathogens.
- Reduce or eliminate alcohol. Avoid drinking too much alcohol to keep your immune system healthy.
While there is no quick fix for pneumonia, following these common-sense prevention tips can help you avoid it. If you do develop pneumonia, a healthy lifestyle will help you recover from it more quickly.
Get the Lowest Price for All Your Medications
BidRx makes it easier for you to fill your prescriptions at the best price. After you request a bid for your medications, pharmacies will bid on your prescription. You can then select the best offer for delivery or local pickup. Place your bid today!
